MTB usually spreads when aerosols from an infected individual pass into the lung of a new host, resulting in one of three possible outcomes8. First, up to two-thirds of people heavily exposed to TB prove to be resistant; they never show any sign of infection9. Second, in other people, the bacilli survive and multiply enough to elicit a long-lived adaptive immune response, reflected in a persistently positive PPD test. The majority of these individuals also harbor resistance to TB, as 90% will never develop active disease. They remain asymptomatic and are said to be latently infected. Finally, 5-10% of infected individuals develop active TB; about half of these individuals present with active TB within one year of exposure, whereas the rest remain asymptomatic for years before developing active disease. Insight into factors that determine which outcome an exposed individual follows would be invaluable for informing new interventions to combat TB.
During the progression to active disease, Mycobacterium tuberculosis (MTB) interacts with and infects a variety of host cell types, and experiences a complex mix of environmental signals – and how the bacterium responds and adapts to these signals in vivo is poorly understood. This proposal tests the concept that behaviors of host and pathogen are coordinated by interwoven regulatory networks, and that the outcome of infection (bacterial containment or active disease) is the product of many network-network interactions that vary both spatially and temporally. If so, it follows that the amplitude and timing of specific network responses will materially alter disease progression – and that perturbing specific networks will both illuminate the topology of the larger network and allow us to define the steps and components critical to infection outcome.
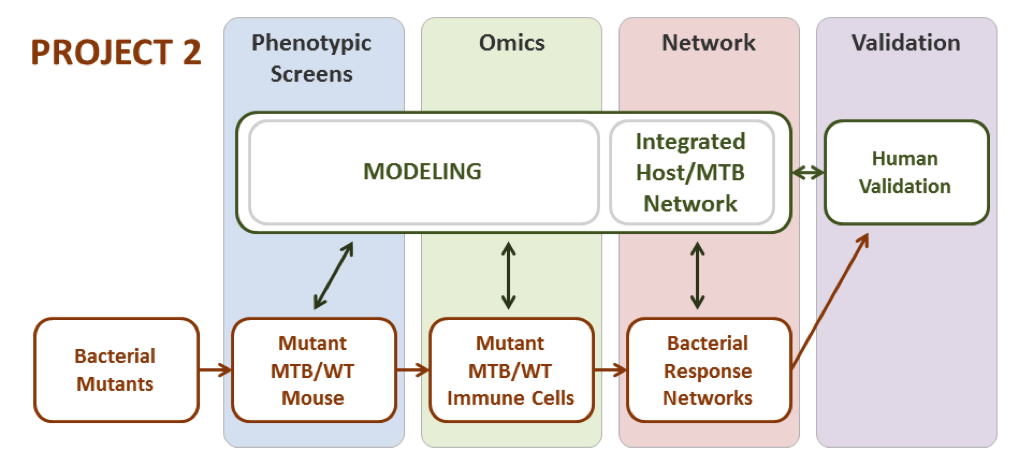 Project 2 will apply systems approaches to dissect the complex problem of TB disease progression in vivo, a first for the field. We first describe an innovative screening strategy to identify the MTB genes critical for disease progression in the lung. Previously we built a DNA binding/gene expression model that allows us to predict a regulon for every MTB transcription factor, and assembled a unique collection of MTB strains in which expression of every regulator is perturbed. We will use these strains to perturb every MTB gene regulatory network during aerosol infection of mouse lungs. Once key regulators are identified, we will quantitate and characterize the changes in infected cell types and determine the specific points in disease progression where particular mutants show altered responses. We then perform detailed systems analysis of the key genes and their predicted regulons using bone marrow macrophages infected ex vivo. We will collect host and MTB transcriptomes, MTB global protein level changes and condition-specific ChIP-seq on key MTB regulators from within matched samples of infected macrophages. These data will fuel modeling of both the bacterial and host response networks, predictions from which will drive a new round of mutant evaluation, omics-scale data collection and additional modeling. Our ultimate modeling Aim, a novel integrated host/MTB network model will be tested using samples from humans, with both candidate mutant bacteria and specific host genes modulated by siRNA.
Project 2 will apply systems approaches to dissect the complex problem of TB disease progression in vivo, a first for the field. We first describe an innovative screening strategy to identify the MTB genes critical for disease progression in the lung. Previously we built a DNA binding/gene expression model that allows us to predict a regulon for every MTB transcription factor, and assembled a unique collection of MTB strains in which expression of every regulator is perturbed. We will use these strains to perturb every MTB gene regulatory network during aerosol infection of mouse lungs. Once key regulators are identified, we will quantitate and characterize the changes in infected cell types and determine the specific points in disease progression where particular mutants show altered responses. We then perform detailed systems analysis of the key genes and their predicted regulons using bone marrow macrophages infected ex vivo. We will collect host and MTB transcriptomes, MTB global protein level changes and condition-specific ChIP-seq on key MTB regulators from within matched samples of infected macrophages. These data will fuel modeling of both the bacterial and host response networks, predictions from which will drive a new round of mutant evaluation, omics-scale data collection and additional modeling. Our ultimate modeling Aim, a novel integrated host/MTB network model will be tested using samples from humans, with both candidate mutant bacteria and specific host genes modulated by siRNA.
